Stanford Law’s Michelle Mello on California’s COVID-19 Spike and Measures to Bend the Curve

On Thursday, June 25, 2020, California saw its biggest spike in COVID-19 cases since the pandemic began in March, with more than 7,000 new cases confirmed. The increase in confirmed cases comes after citizens have endured months of shelter in place orders, the toll has on the health and financial security of millions steep. Why are cases spiking and what can be done to bend the curve of the pandemic in California? Here, Stanford Law Professor Michelle Mello answers these and related questions.
Was California’s “shelter-at-home” (SAH) order effective at flattening the curve of COVID-19? Projections for the state were very gloomy in early March. But we did not hit the worst-case scenarios and the outlook for the state seemed good back in early May.
There is considerable evidence that shelter-at-home and business closure orders, though very burdensome on people and the economy, were successful in flattening the curve. You can see that just by looking at data plots like these that show cases slowing as states implemented orders beginning in late March. There have also been several well-designed studies using mobility data from cellphones that have linked these orders to lower mobility and reduced COVID-19 cases and deaths. From a research perspective, the fact that states and counties entered different orders at different times created a natural experiment that has allowed researchers to isolate the effects of the orders.
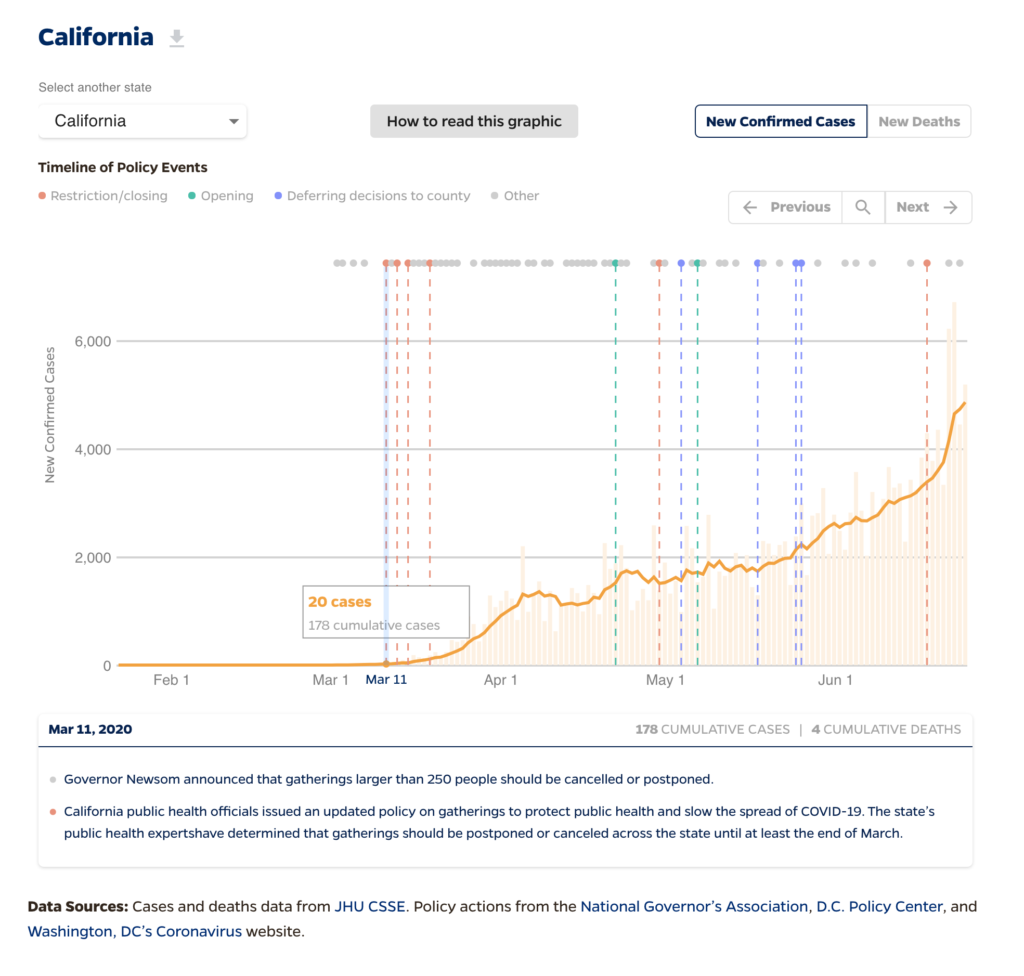
Does the recent surge in cases correlate with the state’s opening up from SIP?
Controlled studies haven’t yet examined the reopening period, but the data certainly point in that direction. Because the Bay Area has maintained its health orders longer than the state’s other large metropolitan area, Los Angeles, there is natural variation within California that researchers will undoubtedly exploit to try to confirm that. Comparing case counts and hospitalizations in those two areas is quite striking.
What do you think is driving the recent spike in cases? Is there any evidence that protests across the state had an effect? Or might it be cabin fever, as Governor Newsom has suggested—that people just started to break the rules and socialize too much? Did increased testing play a role?
We don’t yet have a great handle on all the contributing factors in California, but one thing is clear: it doesn’t merely reflect increased testing, because we’re seeing big increases in the number of hospitalizations (spikes in deaths will likely follow within 1-2 weeks). It has been surprising that the cases during this resurgence have come not only from the anticipated settings, like nursing homes, prisons, and high-density worksites, but also unexpected quarters. A lot of them are young people. Many people have no idea where they contracted the virus; others can point to in-home social gatherings. This suggests it may be a phenomenon of general community spread spurred by people’s lack of adherence to distancing and face covering measures in their social interactions. I haven’t seen any evidence that would link cases specifically to the protests, but it’s still early. There have been some case reports of that in other states.
Another concerning aspect of the resurgence is the concentration of recent cases among Latinx residents in California and elsewhere. A possible explanation is their higher representation among essential workers and lower representation in occupational groups that can work from home. This may not fully explain why cases have spiked in this population during California’s reopening, since many essential workers have been on the job throughout the pandemic; however, workers may be coming into contact with more members of the public since shelter-at-home has been lifted. More contact tracing is required to understand what role social versus on-the-job contacts are playing.
Governor Newsom introduced a statewide mandate for face coverings on June 18.
Do you expect that measure to make a difference?
Although it took a while for the evidence to accrue, at this point “there’s no doubt” that masks “make a difference,” according to Dr. Tony Fauci, and everyone should wear them when they’re around others. They are not a license to congregate, though, because they’re not perfectly protective. Social distancing is still needed. And, we know that not everyone is willing to wear masks. Orders only help if people follow them.
California has a strong antivaxxer movement. Could that be driving the rise? Or associated misinformation and mistrust of science?
It hasn’t helped that people have spread misinformation about COVID-19 on social media and stoked resistance to social distancing measures, and some anti-vaxxers have been among those involved in that. It’s also, of course, very unlikely that these individuals will be willing to accept a SARS-CoV-2 vaccine. But we can’t blame the rebound in cases on them. Nor will it be immediately salient that they’re not willing to be vaccinated. Because so many people will want vaccines when they become available, the question in the near to medium term is not must everyone get them, but who gets to access them? Down the road, a vaccination mandate for high-risk groups might become appropriate, but several conditions would need to be met for that to be the case, as I describe in a June 26 article in the New England Journal of Medicine.
What do you think needs to be done to get control of the virus? Do we need a second SAH—particularly in the counties seeing the biggest spikes including Ventura, Orange, San Bernardino and Riverside counties? Or can masks combined with testing and contact tracing bring this under control?
We don’t have good evidence about whether less restrictive alternatives to a complete shelter-at-home order—meaning wearing masks and keeping 6 feet apart—would be effective enough to get transmission back under control if everyone practiced them consistently. We know not everyone does that. We also know we don’t have the ability to do traditional contact tracing for everyone given the number of cases and the fact that the virus spreads through very casual contact and for a few days before people develop symptoms. But certainly, mass testing and tracing have to be a big part of the endgame.
People tend to think about “lockdown” as a switch that states flip on and off. It’s more useful to think of community mitigation measures as a dial that can be tuned right and left as the epidemiologic situation changes. In between “don’t leave your house” and “do whatever you want” are restrictions on the number of people who can congregate at what time; what activities people may pursue and in what settings; what types of businesses can be open; and so on. States that are seeing cases go in the wrong direction are more likely to “dial up” than to completely revert to a lockdown. For example, Texas just shut bars back down and reduced maximum occupancy at restaurants.
If Californians want to avoid this outcome, what they need to do is simple: stay several feet away from others, wear a mask whenever you’re around others, avoid indoor gatherings, and wash your hands frequently and properly. It’s simple, but not easy. We need to be patient in getting back to some activities that are just not consistent with this advice, like going out to a crowded bar or having a house party. Fortunately, many of the things that need to be postponed indefinitely are things we can live without. If we can do that, we can continue to do more important things: keeping most businesses open and getting people back to work.
Michelle Mello, Professor of Law and Professor of Health Research and Policy (School of Medicine), is a leading empirical health scholar whose research is focused on understanding the effects of law and regulation on health care delivery and population health outcomes. She was elected to the National Academy of Medicine (formerly known as the Institute of Medicine), one of the highest honors in the fields of health and medicine, in recognition of outstanding professional achievement and commitment to service.
